
Assessment of breast symmetry in breast cancer patients undergoing therapeutic mammaplasty using the Breast Cancer Conservation Therapy cosmetic results software (BCCT.core)
Introduction
Therapeutic mammaplasty (TM) is one of the most versatile techniques in oncoplastic breast surgery (OBS). Breast cancer resection is completed followed by reconstitution of breast shape employing breast reduction or mastopexy techniques (1). TM is often performed with simultaneous contralateral balancing surgery in order to maintain symmetry. These immediate symmetrising procedures are advantageous in improving overall patient satisfaction (2), which has been demonstrated to improve the patient’s quality of life (3). An evaluation of outcomes and refinements in the technique of TM over 20 years [1994–2015] by the Emory University group comparing early and more recent cases showed that the technique is effective and increases patient satisfaction (4). A key advantage of TM is that it achieves significantly lower positive margin rates due to the wider excision and can be more successful in obtaining oncological clearance with less re-excisions compared with standard breast conserving surgery (BCS) (5). Its indications include anticipated poor cosmetic outcome with standard BCS, tumours in large and often ptotic breasts, as an alternative to mastectomy and the prevention of lymphedema, fibrosis and chronic pain sometimes associated with irradiating large breasts (6).
Although TM is well established there is a paucity of literature pertaining to the objective analysis of its aesthetic outcomes (6-8). Hence it was the aim of this study to compare objective and subjective evaluations of the cosmetic outcomes of patients who had undergone TM in the Cambridge Breast Unit (CBU). This was assessed objectively using the Breast Cancer Conservation Treatment cosmetic results software (BCCT.core) and subjectively using a panel of surgeons.
The BCCT.core is a validated evaluation tool for analysing cosmetic outcomes following standard BCS (8-12). It assesses breast asymmetry, skin colour difference and scar visibility (13). The software has previously been applied to evaluate outcomes following standard wide local excision (WLE) (10,14), and very recently following TM for upper pole breast tumours (15). However, until now it has not been used to assess tumours in all locations within the breast. We aimed to establish its use for such tumours by comparing results with subjectively obtained data using pre- and post-operative photos. Subjective data were obtained from ratings of a plastic surgical panel using a Visual Analogue Scale (VAS) to assess the photographs.
Methods
Twenty patients were identified that had had therapeutic mammaplasties performed jointly with the same oncologic breast surgeon performing the WLEs and any necessary axillary surgery. All resections were assessed by intraoperative X-ray and additional tissue taken as indicated. Prior signed informed consent was obtained from all the patients for evaluation of their anonymised photographs. Electronic and paper clinical records were reviewed to identify relevant clinico-pathological features namely patient demographics, tumour and treatment characteristics. These included pre-operative investigations, surgery techniques & pedicles used, tumour location & size, resection weights, excision margins and post-operative radiotherapy (RT) received.
Standardised photographs of 20 patients both pre-operatively and at a median of 7 months post-operatively were taken by a dedicated medical photographer. All patients were photographed in frontal, both lateral and both oblique positions with their arms behind their backs using the same source of lighting and distance from camera in order to avoid any differences in skin colour and angle. For breast symmetry assessments, only anterior-posterior (AP) views were used.
Objective assessment required pre- and post-operative frontal-view photographs to be loaded into the BCCT.core software program with the following landmarks being digitally marked: nipples, suprasternal notch and the most medial and lateral points of the breasts. The software then automatically adjusted the outline of the breast contour and generated the final cosmetic result, classified as 1 of 4 categories, i.e., excellent, good, fair, poor (Figure 1), based on the Harvard Scale introduced by Harris in 1979 (16). The results for both the pre and post-operative photographs were then compared.
Subjective analysis was conducted by anonymised photographs being presented to the panel which consisted of 16 members. They were shown both pre- and post-operative frontal views of the 20 patients. Each member of the panel then scored the breasts using size and shape symmetry criteria on the 10-point VAS. The data were compiled on an excel spreadsheet and the mean score for each patient calculated. In order for results to be comparable to the objective assessment, the score was then re-categorised (0 to <2.5, 2.5 to <5, 5 to <7.5, 7.5–10) to correspond to the BCCT.core scoring (poor, fair, good, excellent).
Results
General
A total of 20 patients who underwent 22 TMs were reviewed. Their mean age was 51.5 years (range, 37–63 years). Ninety-four percent of patients received adjuvant RT. The indications for the TM were invasive breast cancer (87%) and ductal carcinoma in situ (DCIS) (13%). Tumour size ranged from 6 to 90 mm (median 22.5 mm), the median resection weight was 245.8 g (range, 16–1,079 g) and the median closest margin was 8 mm. The majority of tumours were invasive carcinoma of no special type (NST) (56.5%), followed by DCIS (13%), mixed NST + DCIS (17.4%), mixed lobular + NST (8.7%) and lobular (4.4%).
Most tumours were located in zone 6 of the breast (39%) followed equally by zone 4 and 7 (18%). Primary nipple pedicles for the lumpectomy defects were; superomedial (63%), inferior (21%) and superolateral (16%). Five patients had a secondary pedicle to facilitate parenchymal redistribution to optimise breast reshaping and maintenance of a satisfactory contour. Three patients had a Grisotti style rotation-advancement flap to recreate an areola.
Axillary surgery concurrently done was performed through the breast incision in 13/18 cases [7 clearances, 11 sentinel lymph node biopsies (SLNB)]. The remaining four cases had upfront SLNB prior to neoadjuvant chemotherapy or completion clearance for a positive SLNB.
The pedicle technique used for simultaneous contralateral balancing mammaplasty was the same as for the index breast in 75%. Contralateral breast tissue resection weights ranged from 59 to 1,366 g (median 610 g) and were all benign. No revision operations were requested nor required in the index breasts and no further balancing surgery was performed on the opposite breast.
One out of the 20 patients had a complication (5% complication rate) consisting of T-junction wound breakdown accompanied by fat necrosis. She however did not require adjustment procedures. One patient did not attend for post-operative photographs so her images could not be analyzed on BCCT.core or by the panel.
Objective assessment by BCCT.core
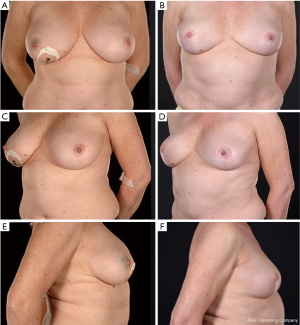
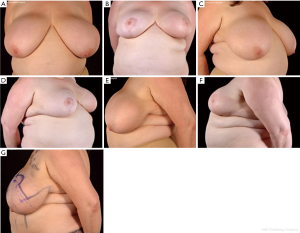
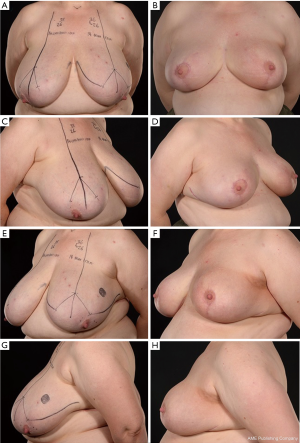
Thirty-seven percent (n=7) of the patients achieved excellent scoring post-operatively (Figures 1,2) and 63% (n=12) achieved good symmetry (Figure 3). Post-operative breast symmetry improved from good to excellent in 37% of breasts (n=7) (Figure 2), whilst for 16% (n=3) of patients the symmetry reduced from excellent to good (Figure 3). In the remaining patients, the score was maintained as excellent or good.
Subjective assessment by panel
When frontal-view post-operative breast symmetry was assessed by the panel, it was rated as excellent in 32% (n=6) of patients, good in 58% (n=11) and fair in 10% (n=2). Twenty-one percent of these scores were an improvement on the pre-operative appearances, 69% of scores were maintained, and 10% were reduced. In the oblique photos, the 15% (n=3) were classed as excellent and 85% (n=16) as good; with 15% being an improved score, 5% a reduction and the rest maintaining their scores.
Oncological outcomes
Two patients had positive resection margins (10% re-excision rate). One had extensive invasive lobular cancer, grossly underestimated on preoperative MRI and went on to a completion mastectomy and deep inferior epigastric artery perforator (DIEP) flap immediate reconstruction. The other was for DCIS and she underwent mastectomy and implant-based reconstruction. There have been no recurrences in any of the 20 patients to date.
Comparison of BCCT.core to panel assessment
Analysis using the Wilcoxon matched-pairs signed rank sum test found that the comparisons between objective and subjective ratings found no difference between them on the pre-operative (P=0.70) or post-operative (P=0.30) appearances. Similarly, when the two groups were combined (pre-op + post-op scores) there was no significant difference between the objective and subjective assessments signifying a high concordance rate between them.
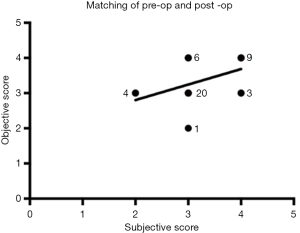
To assess similarity, Spearman rank order tests found that the objective and subjective ratings for the pre-operative photos were significantly similar (P=0.003, rs =0.57). It also found the two ratings for the post-operative photos to be significantly similar (P=0.02, rs =0.45). When grouping together all photos, assessments of pairing effectiveness found that subjective and objective scoring were significantly similar (P=0.0004, correlation coefficient r=0.50) (Figure 4).
Discussion
TM has evolved to become a versatile tool to facilitate BCS while preserving the breast form. Oncoplastic BCS where appropriate is preferable to mastectomy as it has been shown to be as oncologically safe as mastectomy when combined with RT, but leaves the patient with a sensate breast.
The Wise pattern was the most common skin excision technique because of its versatility in allowing use of different dermoglandular pedicles (17). Additionally, for large breasts, as were most of the breasts in our study (median cup size: 36G), it facilitates generous tissue and skin excision resulting in a better aesthetic outcome (18). TM requires that the surgeon is well versed in all breast reduction techniques. This was demonstrated in the variation of our series where superomedial, superior, superolateral, inferior and central pedicles were used, as were different combinations with non-nipple bearing (such as the Grisotti flap), nipple-bearing or nipple-transposing pedicles.
TM is effective in maintaining breast cosmesis and often even enhancing it. This has been demonstrated by objective assessment, using BCCT.core software which aims to standardise aesthetic evaluation after BCS. When compared to subjective evaluation using a 10-point VAS there was a significant concordance of the results in paired matching statistical tests. The panel and BCCT.core assessments rated the aesthetic outcomes as good or excellent in the majority of cases, reflecting the TMs effectiveness for breast cosmesis in general and breast symmetry in particular.
Interestingly, the panel was more critical of the outcomes as they rated two patients (1 in 10) as only fair. However, when comparing differences between pre- and post-operative photos, both objective and subjective scoring systems showed congruent results, with similar values for improving, maintaining and reducing cosmesis. BCCT.core was therefore very useful for objectively assessing cosmesis and, despite the small patient numbers, gave comparable findings with the panel, thus suggesting the validity of BCCT.core for all breast zones. These positive aesthetic results would have been achieved through joint plastic and oncological breast surgical meticulous pre-operative planning and marking of skin paddles to guide excisions and joint intraoperative execution of the surgical plans.
Our series has shown that it is possible to remove large tumours in large breasts with good margins using oncoplastic techniques. These cases would have traditionally been treated by mastectomy. Studies have shown that patient-reported outcome measures (PROMs) are better in BCS compared to mastectomy (19,20). In addition in those patients with large ptotic breasts breast reduction has been associated with high patient satisfaction and therefore it is understandable that both the panel and BCCT software have in some cases demonstrated an improvement in cosmesis post-surgery (21).
A limitation of our study was the relatively small sample size, but despite this, satisfactory results were obtained, both subjectively and objectively. The BCCT.core software, whilst being an objective, innovative and reproducible tool, uses only frontal-view 2D photographs. This limits its ability to evaluate the depth, projection and breast volume which would require 3D visualisation. However, since the BCCT.core bases its results on skin colour and scar visibility in addition to breast symmetry, it may combine sufficient information to give accurate applicable results (8).
TM is effective in achieving good oncological and cosmetic outcomes in both small and large resections during BCS for cancer. Achieving clear margins with minimal morbidity in selected breast cancer patients ultimately results in very favourable overall clinical and aesthetic results. The BCCT.core software is a useful objective tool in the simple and accurate analysis of post-operative results in patients undergoing TM. Our study validates that its use was comparable to a subjective analysis using the VAS tool by a team of 16 specialty doctors.
Conclusions
We demonstrated the feasibility of BCCT.core software use in TMs for cancers in all breast locations having compared this with a plastic surgical panel. Notwithstanding the small patient numbers, the software results were comparable with findings of the panel. This suggests validity of BCCT.core for all breast zones.
Acknowledgments
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was a service evaluation project within the Department of Plastic and Reconstructive Surgery at the Cambridge Breast Unit. Service evaluation projects are part of a larger framework for Clinical Governance, whereby National Health Service (NHS) organizations are accountable for continuously improving the quality of their services and safeguarding high standards. Clinical governance (inclusive of service evaluation projects) is compulsory within the NHS. No ethical committee approval is needed. Under the Caldicott Principles, nonidentifiable patient data can be collected, stored and used for purpose of audit without individual patient consent. Additionally, all data were collected retrospectively from hospital medical records. Therefore, individual patient consent was not required for this study. Subjects in clinical photographs gave informed consent for use of images in journal publication.
References
- Macmillan RD, McCulley SJ. Oncoplastic Breast Surgery: What, When and for Whom? Curr Breast Cancer Rep 2016;8:112-7. [Crossref] [PubMed]
- Urban C, Furlan Anselmi K, Kuroda F, et al. Oncoplasty as the Standard of Care in Breast Cancer Surgery. European Oncology & Haematology 2014;10:43-7. [Crossref]
- Waljee JF, Hu ES, Ubel PA, et al. Effect of esthetic outcome after breast-conserving surgery on psychosocial functioning and quality of life. J Clin Oncol 2008;26:3331-7. [Crossref] [PubMed]
- Losken A, Hart AM, Broecker JS, et al. Oncoplastic Breast Reduction Technique and Outcomes: An Evolution over 20 Years. Plast Reconstr Surg 2017;139:824e-833e. [Crossref] [PubMed]
- Campbell EJ, Romics L. Oncological safety and cosmetic outcomes in oncoplastic breast conservation surgery, a review of the best level of evidence literature. Breast Cancer (Dove Med Press) 2017;9:521-30. [Crossref] [PubMed]
- McIntosh J, O'Donoghue JM. Therapeutic mammaplasty--a systematic review of the evidence. Eur J Surg Oncol 2012;38:196-202. [Crossref] [PubMed]
- Iwuchukwu OC, Harvey JR, Dordea M, et al. The role of oncoplastic therapeutic mammoplasty in breast cancer surgery--a review. Surg Oncol 2012;21:133-41. [Crossref] [PubMed]
- Cardoso MJ, Oliveira H, Cardoso J. Assessing cosmetic results after breast conserving surgery. J Surg Oncol 2014;110:37-44. [Crossref] [PubMed]
- Preuss J, Lester L, Saunders C. BCCT.core - can a computer program be used for the assessment of aesthetic outcome after breast reconstructive surgery? Breast 2012;21:597-600. [Crossref] [PubMed]
- Heil J, Carolus A, Dahlkamp J, et al. Objective assessment of aesthetic outcome after breast conserving therapy: subjective third party panel rating and objective BCCT.core software evaluation. Breast 2012;21:61-5. [Crossref] [PubMed]
- Haloua MH, Krekel NM, Jacobs GJ, et al. Cosmetic Outcome Assessment following Breast-Conserving Therapy: A Comparison between BCCT.core Software and Panel Evaluation. Int J Breast Cancer 2014;2014:716860. [Crossref] [PubMed]
- O'Connell R, Di Micco R, Dean S, et al. Correlation of BCCT.core objective scoring software for aesthetic outcome after breast conservation with panel assessment and patient satisfaction. Eur J Surg Oncol 2017;43:S9. [Crossref]
- Cardoso MJ, Cardoso J, Amaral N, et al. Turning subjective into objective: the BCCT.core software for evaluation of cosmetic results in breast cancer conservative treatment. Breast 2007;16:456-61. [Crossref] [PubMed]
- Yu T, Eom KY, Jang NY, et al. Objective Measurement of Cosmetic Outcomes of Breast Conserving Therapy Using BCCT.core. Cancer Res Treat 2016;48:491-8. [Crossref] [PubMed]
- Hashem T, Farahat A. Batwing versus Wise pattern mammoplasty for upper pole breast tumours: a detailed comparison of cosmetic outcome. World J Surg Oncol 2017;15:60. [Crossref] [PubMed]
- Harris JR, Levene MB, Svensson G, et al. Analysis of cosmetic results following primary radiation therapy for stages I and II carcinoma of the breast. Int J Radiat Oncol Biol Phys 1979;5:257-61. [Crossref] [PubMed]
- McCulley SJ, Macmillan RD. Planning and use of therapeutic mammoplasty--Nottingham approach. Br J Plast Surg 2005;58:889-901. [Crossref] [PubMed]
- Choo AM, Forouhi P, Malata CM. Innovative combination of therapeutic mammoplasty and expandable-implant breast augmentation for immediate partial breast reconstruction. Int J Surg Case Rep 2016;23:146-50. [Crossref] [PubMed]
- Di Micco R, O'Connell RL, Barry PA, et al. Bilateral mammoplasty for cancer: Surgical, oncological and patient-reported outcomes. Eur J Surg Oncol 2017;43:68-75. [Crossref] [PubMed]
- Chand ND, Browne V, Paramanathan N, et al. Patient-Reported Outcomes Are Better after Oncoplastic Breast Conservation than after Mastectomy and Autologous Reconstruction. Plast Reconstr Surg Glob Open 2017;5:e1419. [Crossref] [PubMed]
- Currie A, Chong K, Davies GL. Using therapeutic mammoplasty to extend the role of breast-conserving surgery in women with larger or ptotic breasts. Ann R Coll Surg Engl 2013;95:192-5. [Crossref] [PubMed]


