Management of gynecomastia—changes in psychological aspects after surgery—a systematic review
Introduction
Gynecomastia is the benign enlargement of glandular breast tissue in men. It is usually caused by increased estrogen activity, decreased testosterone activity, or the use of numerous medications (1). It usually debuts during adolescence and it is reported in up to 65% of the male population (2,3).
After the cause of gynecomastia has been identified, treatment usually involves either medical or surgical intervention.
Regarding surgical treatment, there are many different techniques, mainly consisting of liposuction, gland excision or a combination of both. Surgical treatment for gynecomastia is generally not recommended in the first year of symptoms, especially as there is a chance of spontaneous resolution of the problem (4,5).
Though surgery may be effective in correcting the cosmetic aspect of gynecomastia, research has indicated that the psychological factor may be significant in these patients.
In 1961 Schonfeld published an article suggesting that gynecomastia’s impact on a man’s life warranted both surgical treatment and psychotherapy (6).
The subsequent research performed on the correlation between the psychological effects of gynecomastia and how surgical treatment affects these have been limited. Studies performed on adults and adolescents, with gynecomastia, have reported significant negative impact on psychosocial aspects, such as well-being, social functioning, mental health and self-esteem (7,8). The main theory behind this correlation is that at the age of adolescence children solidify their body image, self-esteem and sexual identity. The abnormal development of the breast tissue could, in this period, impact these domains and be an anatomic stressor (9). In a study by Li et al., 94.8% of patients reported psychological stress because of their gynecomastia (10).
Research performed on the treatment of gynecomastia has largely focused on surgical intervention and how effective it is at correcting the enlarged breast. In these articles, the focus on the patient’s perspective has been scarce, mostly reporting on patient satisfaction by a simple 1–10 scale. A comprehensive review published in 2015, by Fagerlund et al., found high satisfaction rates in patients surgically treated for gynecomastia. Only two, of their included articles, reported on other parameters than, patient satisfaction alone (11). When investigating the psychological impact of surgical intervention there is, arguably, a need for a more multifaceted evaluation. During the last years, several papers have investigated the psychological impact of gynecomastia and what effect surgical treatment has the different psychological domains in these patients. Understanding the psychological aspect of this disease could improve patient care, especially when trying to identify the patients that will benefit from treatment.
This systematic review summarises the published data on the psychological effect of surgical treatment for gynecomastia.
Methods
This systematic review and meta-analysis was conducted using the well-recognised methodology and reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement (12).
Eligibility criteria
Studies reporting on psychological outcomes after surgical intervention for gynecomastia were included. Only articles in the English language were eligible for inclusion and there was limitation on date of publication within the last 10 years.
Information sources and search strategy
A computerised search was performed using MEDLINE, OVID, Cochrane Library and Cinahl. The last search was performed 25.04.17. Reference lists of identified studies and previously published reviews were also explored. The search was performed using the terms “gynecomastia” and “surgery”. The search was restricted to articles published within the last 10 years. All searches were supplemented by an additional free word search. The specific search strategies can be seen in Table S1.
Full table
Study selection and data-collection process
A database search was used to identify eligible citations. Duplicates were removed and the studies were evaluated on title and abstract. This was followed by full-text assessment, identifying the included studies. From these studies, data on the number of cases and their characteristics, type of psychological measurement tool, and other outcome measures were extracted.
Risk of bias in individual studies
The included articles were evaluated on the risk of bias, using the Cochrane Risk of Bias Assessment Tool (13). Domains evaluated were selection bias, performance bias, detection bias, attrition bias, reporting bias and other bias. Each domain was deemed “low risk of bias”, “intermediate risk of bias” or “high risk of bias”. “Low risk of bias” was given to the articles who were thoroughly discussing their article in relation to the specific bias. “Intermediate risk of bias” was given to those who were not specifically stating how the bias affected their results, but where we, as readers, could evaluate this by interpreting text and data. “High risk of bias” was given to the articles where an evaluation of the bias could not be made sufficiently.
Synthesis of results
This systematic review was performed using the Covidence software, developed and supported by the Nordic Cochrane Centre (14). The Covidence database enables a faster and more secure review as it allows for duplicates to be removed, data to be stored and makes the review process transparent and more organised.
Results
Study selection
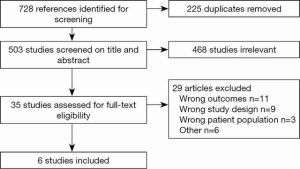
The database search identified 728 citations. Duplicates and non-eligible types of publications were removed and 503 studies were evaluated on title and abstract. Twenty-nine studies were eligible for full-text assessment. After full-text review, six studies were included in this review (Figure 1).
Study characteristics
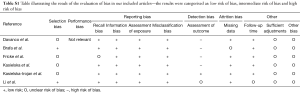
Characteristics of the included studies can be found in Table 1. Four of the studies were case-control studies and two were retrospective cohort studies. The studies originated from Brazil, Italy, Germany, Taiwan, and Poland. Two of the studies had the same first author. The studies were all published between 2009 and 2017. The number of cases in these studies ranged from 16 to 126. The mean age ranged from 25.0 to 32.4. Four of the included studies assessed psychological domains pre-operatively and post-operatively (8,10,15,16). The follow-up time ranged from 3–12 months after surgery. Fricke et al. investigated long-term satisfaction/quality of life after surgery and interviewed patients only post-surgery, with a mean follow-up time of 13.8 years (17).

Full table
All included articles reported on outcomes relating to patients quality of life. They did not use the same measurement tool. Two studies used the 36-item short form survey (SF-36), reporting on quality of life measures (8,15). Kasielska-Trojan et al. also added two extra questions, one about the effect of gynecomastia on personal life and one investigating whether or not undergoing surgery was a good decision (15). The study by Fricke et al. used the consultant satisfaction questionnaire (CSQ-9) when assessing changes in patients psyche (17). Two studies used questionnaires developed by the authors, investigating domains known to be problematic for their patients (10,16).
The intervention in all included articles consisted of liposuction, adenectomy or a combination of both. The studies varied in reporting the exact method of subcutaneous mastectomy used.
The risk of bias within and across studies
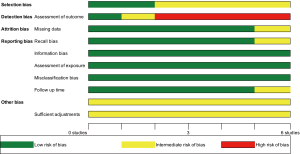
The assessment of the risk of bias can be seen in Table S1. The included studies were generally good at reporting bias. No study reported on adjustments being done to their statistical analysis. Three studies also lacked information on whether or not patients invited to participate in their study was a selected group or all patients undergoing surgery (15-17). A summary of the assessment of the risk of bias can be seen in Figure S1.
Results of the individual studies
Results of the individual studies can be seen in Table 2.

Full table
Psychological domains
Two studies used the SF-36 as the assessment tool. One of these, Kasielska-Trojan et al. found a statistically significant improvement in the following domains; functional capacity, limitations due to physical aspects, limitations due to pain, general health, vitality, social aspects, limitations due to emotional aspects and mental health/well-being (15). The other study, Davanço et al., observed the same tendency, except for; limitations due to physical aspects, limitations due to emotional aspects and limitations due to pain, where no improvement was seen (8). Kasielska-Trojan et al. also found a statistically significant increase in assessment of personal life after surgery (15).
Fricke et al observed improved self-esteem in all age groups, with a tendency of bigger increase in younger patients (17). Li et al. observed high self-confidence levels after surgery in their patients with a score of >9/10 (10).
Brafa et al. found an improvement in the Quality of Life of all patients, with a tendency of larger improvement in those with the more severe gynecomastia (18).
Kasielska et al. observed a statistically significant improvement in the following domains; emotional discomfort, difficulties with relationships with women, limiting everyday activity, failures in life, ridiculing by others, feelings of isolation, embarrassment when talking about their problem and personal life assessment (16).
Discussion
Summary of evidence
This systematic review identified several psychological domains affected by gynecomastia. The published data on the effect of surgical treatment on these domains, suggests that patients, in general, experience improvement their psychological health. The amount of published data is limited and the quality is very low. Caution should be taken when concluding on this material.
Assessment of the psychological impact of gynecomastia
The evaluation tools for assessing the effect on psychological domains are different across all our studies. This makes a direct comparison across all studies impossible, which is problematic. Two studies applied the SF-36 (8,15). The SF-36 has been used for decades and is recognised as a valid and comprehensive assessment tool when estimating the relative burden of different medical conditions (19). Fricke et al. used the CSQ-9 as the assessment tool (17). The CSQ-9 was developed around 1990 as a tool for evaluating patients satisfaction with medical consultations (20). It is mostly used in the primary care sector (21).
Brafa et al. used a simple 1–10 scale do assess the quality of life (18). Though it is convenient to use such a short evaluation tool, it could potentially be problematic as the data on the different aspects of quality of life is very limited.
Two studies used questionnaires developed by the authors to evaluate psychological domains (10,16). The advantage of this method is the possibility of getting information about the exact domain being investigated. A review by Edwards concluded that a good questionnaire design would minimise bias and maximise precision in the estimates of treatment effect. He also concluded that as questionnaire design is as much an art as a science, there are risks accompanied by their development (22). When interpreting the results of these studies this possible source of bias needs to be taken into consideration.
The large variation in assessment tools in the included articles could indicate that there is a need for a more specific, validated tool for this patient group. This is supported by a comprehensive review by Clapham et al. that investigated the use of patient scores in plastic surgery research. Their conclusion was; that the scarcity of patient reported outcome research in craniofacial, hand, and other reconstructive specialties, as well as the use of invalidated instruments, are current barriers preventing plastic surgery patient reported outcome studies from producing meaningful results (23). In this review, the articles using the validated assessment tool SF-36 has been given the most weight when comparing results.
Study populations
Regarding selection bias in the retrospective studies, most have not stated if the included population is a selected one, or if all patients treated in the time period was included. This is a possible source of bias.
The mean age of the population included in this review is around 25 years old. This is low considering that gynecomastia is a disease affecting all age groups. The prevalence of gynecomastia is up to 70% in men aged 50 to 69 years (24). Our results, when summarizing the findings of our included articles, will therefore not represent this age group.
Surgical methods across studies
The method of surgery also varies across studies. They are all based on the surgical approach of adenectomy and liposuction. Though all articles describe different sub-categories of surgery, they are, in the author’s opinion a reflection of the diversity in this group of patients, and the articles are comparable. No article reported using a treatment algorithm or other tool to standardise the assignment of surgery type to the individual patient. There is no broad consensus regarding a treatment algorithm for gynecomastia that makes comparing methods of the included studies difficult. Such treatment algorithms have been developed, but are not widely used (11,25,26).
Surgical versus psychological treatment
The question on whether or not gynecomastia warrants surgical intervention has been debated for decades. Braunstein argued that as pubertal gynecomastia resolves with time in the majority of adolescent boys, reassurance and follow-up physical examination usually suffice (5). This is generally accepted and most surgeons would not operate on someone with a short history of gynecomastia.
As gynecomastia is a benign disease and the problem is mostly psychological, one could argue that simply treating the psychological problem is the best solution. Kinsella et al. made a counterargument to this statement with the argument being, that as no amount of counselling will fix the anatomic issue, the therapy would need to be lifelong. Further allowing these patients to persist with the psychological burden of depression and anxiety (along with the attendant risk of suicide and other self-harming behaviors) would be out of line with the best interest of the patient (9). There seems to be a strong link between psychological domains and gynecomastia and both the psychological and physical aspect should, therefore, be considered when treating these patients. They also concluded that surgeons should strongly consider referring their patients with gynecomastia for psychological evaluation and treatment as an adjunct to successful management of this condition (9).
Other
Two studies are by the same first author, which raises the question of biased data material of this systematic review. The two studies are from different periods of time and are based on different patient populations and report on different outcomes. When assessing quality and risk of bias in these two studies they both were evaluated as being of good quality and were therefore included in our study.
The low number of included articles is a limitation of this study. All data published on this topic were evaluated for inclusion. The low number of published studies and the low quality of evidence emphasises the need for further study on this subject.
Conclusions
Surgical treatment of gynecomastia seems to be beneficial for several psychological domains. Among these are vitality, emotional discomfort, limitations due to physical aspects and limitations due to pain. There is a trend of improvement in quality of life and psychological health. The results are, however, based on data for a patient population in their mid-twenties and are therefore not representative of all men affected by gynecomastia.
The quality of evidence is very low and future studies examining the impact of the surgical intervention for gynecomastia on psychological domains are greatly needed. These studies should include data from older individuals affected by gynecomastia and utilise valid tools of psychological measurement in order to better quantify the effect. The older patients affected by the disease have been overlooked in the current research. More data on this subject could improve the pre-operative evaluation of these patients and help identify the patients that will benefit from treatment.
Acknowledgements
None.
Footnote
Conflicts of Interest: The author has no conflicts of interest to declare.
References
- Johnson RE, Murad MH. Gynecomastia: pathophysiology, evaluation, and management. Mayo Clin Proc 2009;84:1010-5. [Crossref] [PubMed]
- Niewoehner CB, Nuttal FQ. Gynecomastia in a hospitalized male population. Am J Med 1984;77:633-8. [Crossref] [PubMed]
- Carlson HE. Gynecomastia. N Engl J Med 1980;303:795-9. [Crossref] [PubMed]
- Thiruchelvam P, Walker JN, Rose K, et al. Gynaecomastia. BMJ 2016;354:i4833. [Crossref] [PubMed]
- Braunstein GD. Clinical practice. Gynecomastia. N Engl J Med 2007;357:1229-37. [Crossref] [PubMed]
- Schonfeld WA. Gynecomastia in adolescence. Personality effects. Arch Gen Psychiatry 1961;5:46-54. [Crossref] [PubMed]
- Nuzzi LC, Cerrato FE, Erickson CR, et al. Psychosocial impact of adolescent gynecomastia: a prospective case-control study. Plast Reconstr Surg 2013;131:890-6. [Crossref] [PubMed]
- Davanço RAS, Sabino Neto M, Garcia EB, et al. Quality of life in the surgical treatment of gynecomastia. Aesthetic Plast Surg 2009;33:514-7. [Crossref] [PubMed]
- Kinsella C, Landfair A, Rottgers SA, et al. The psychological burden of idiopathic adolescent gynecomastia. Plast Reconstr Surg 2012;129:1-7. [Crossref] [PubMed]
- Li CC, Fu JP, Chang SC, et al. Surgical treatment of gynecomastia: complications and outcomes. Ann Plast Surg 2012;69:510-5. [Crossref] [PubMed]
- Fagerlund A, Lewin R, Rufolo G, et al. Gynecomastia: A systematic review. J Plast Surg Hand Surg 2015;49:311-8. [Crossref] [PubMed]
- Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 2009;151:264-9, W64.
- Assessing Risk of Bias in Included Studies, The Cochrane Collaboration. 2018. [Internet]. [cited 2018 Mar 10]. Available online: methods.cochrane.org/bias/assessing-risk-bias-included-studies
- Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at [Internet]. Available online: www.covidence.org
- Kasielska-Trojan A, Antoszewski B. Gynecomastia Surgery-Impact on Life Quality: A Prospective Case-Control Study. Ann Plast Surg 2017;78:264-8. [Crossref] [PubMed]
- Kasielska A, Antoszewski B. Effect of operative treatment on psychosocial problems of men with gynaecomastia. Pol Przegl Chir 2011;83:614-21. [Crossref] [PubMed]
- Fricke A, Lehner GM, Stark GB, et al. Long-Term Follow-up of Recurrence and Patient Satisfaction After Surgical Treatment of Gynecomastia. Aesthetic Plast Surg 2017;41:491-8. [Crossref] [PubMed]
- Brafa A, Campana M, Grimaldi L, et al. Management of gynecomastia: an outcome analysis in a multicentric study. Minerva Chir 2011;66:375-84. [PubMed]
- Ware JE. SF-36 health survey update. Spine 2000;25:3130-9. [Crossref] [PubMed]
- Baker R. Development of a questionnaire to assess patients’ satisfaction with consultations in general practice. Br J Gen Pract 1990;40:487-90. [PubMed]
- Baker R, Smith A, Tarrant C, et al. Patient feedback in revalidation: an exploratory study using the consultation satisfaction questionnaire. Br J Gen Pract 2011;61:e638-44. [Crossref] [PubMed]
- Edwards P. Questionnaires in clinical trials: guidelines for optimal design and administration. Trials 2010;11:2. [Crossref] [PubMed]
- Clapham PJ, Pushman AG, Chung KC. A systematic review of applying patient satisfaction outcomes in plastic surgery. Plast Reconstr Surg 2010;125:1826-33. [Crossref] [PubMed]
- Young CC, Young CC, Rew L, et al. Psychosocial Correlates of Idiopathic Gynecomastia in Young Males: Preliminary Findings From a Mixed-Methods Study. J Adolesc Health 2016;60:S26. [Crossref]
- Cordova A, Moschella F. Algorithm for clinical evaluation and surgical treatment of gynaecomastia. J Plast Reconstr Aesthet Surg 2008;61:41-9. [Crossref] [PubMed]
- Ratnam BV. A new classification and treatment protocol for gynecomastia. Aesthet Surg J 2009;29:26-31. [Crossref] [PubMed]