Adrenal lymphangioma presenting as a non-functional adrenal cyst
Introduction
Cysts of the adrenal gland can be endothelial (45%), pseudocysts (39%), epithelial (9%) or parasitic (7%) in origin (1). The majority of adrenal cysts are benign and non-functional. Functioning and large cysts are known to have a higher risk of malignancy (2). We describe a case of an adrenal lymphangioma which presented as a non-functioning adrenal cyst.
Case history
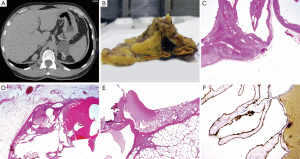
A male patient presented with left scrotal pain in 2012. Ultrasound scan of the scrotum revealed a varicocele. Further upper genito-urinary tract imaging with CT scan showed a 5.5-cm left adrenal mass with calcification (Figure 1A). On investigation adrenal biochemistry was within normal limits with plasma metanephrine levels of 0.20 nmol/L (indicating a very low probability of a pheochromocytoma). Clinically and radiologically the features were those of a non-functional adrenal cyst. As the lesion was large (>5 cm), a decision for excision was undertaken and the patient underwent a left adrenalectomy. Macroscopically, a 5.5 cm × 3.7 cm cyst was identified within the adrenal gland with a multiloculated cut surface and mucoid contents (Figure 1B). Microscopically, thin septae formed the walls of the locules; these were filled with eosinophilic fluid and contained sheets of macrophages (Figure 1C-E). Focal calcification was noted. The locules were lined by flattened endothelial cells which expressed CD31 (Figure 1F) but not CD34, CK7 or CK20, confirming a diagnosis of adrenal lymphangioma. The lesion had been completely excised and required no further treatment.
Discussion
Pathogenetically, lymphangiomas are benign proliferations of vascular origin, histogenetically arising from lymphatic endothelium. They can be developmental or neoplastic. Most are cystic and are composed of dilated lymphatic channels. They occur at all ages but are most frequently seen in children and in the 3rd to 6th decades of life (3). Lymphangiomas are rare in the chest and abdominal cavity with 95% occurring in the neck and axilla. They have extremely rarely been documented in the adrenal gland, with <60 cases reported in literature (4) and account for <1% of all abdominal lymphangiomas (5).
Adrenal lymphangiomas usually remain asymptomatic throughout life, being found incidentally during abdominal imaging studies, surgery or at autopsy. Symptoms if present are usually related to mass effect (pain, gastrointestinal disturbance, or very rarely a palpable mass) (6).
Differentiation of cystic adrenal lymphangiomas from other benign adrenal cysts and adrenal solid tumours with cystic change poses a diagnostic challenge on imaging. Hormonal evaluation is useful in making the distinction (7). Laboratory findings are by and large non-contributory in diagnosing adrenal lymphangiomas. Hormonal evaluation helps to identify the small subset of “functional cysts” of adrenocortical origin. However this does not solve the problem of distinguishing a lymphangioma from non-functional cysts.
Imaging is able to identify the cystic nature of the lesion but it also does not allow one to reliably distinguish between a non-functioning adrenal cyst and an adrenal lymphangioma. On Ultrasound, adrenal lymphangiomas are well-marginated, typically suprarenal, anechoic lesions which can show shadows or echoes when calcifications are present (8). CT usually demonstrates a hypodense, non-enhancing lesion; on MRI, most are low in signal intensity on T1-weighted images and high on T2-weighted images. If haemorrhage occurs in adrenal lymphangiomas, signal intensity changes to high on both T1- and T2-weighted images (8).
On pathological examination adrenal lymphangiomas are multiloculated, thin-walled cystic lesions, filled with non-viscous, clear, yellow-brown coloured fluid. Microscopy demonstrates that the irregular dilated cystic channels/spaces contain proteinaceous material and usually lack red blood cells. They are lined by flattened, simple endothelial cells, which on immunohistochemistry express CD31, D2-40 (a lymphatic endothelial marker) and are negative for calretinin and CD34.
Management of adrenal cysts including lymphangiomas is based on endocrinological and clinical findings. Small asymptomatic non-functioning cysts are treated conservatively. Indications for surgery include large cysts (≥5 cm diameter), certain imaging findings [high density on unenhanced CT (>10 HU), delayed wash-out of the contrast medium, significant growth of the cyst on serial imaging], functional cysts, symptomatic cysts and cysts prone to complications such as hemorrhage, rupture, or infection (2).
While non-functioning cysts of the adrenal gland are not uncommon in clinical practice (due to the ease with which asymptomatic, incidental lesions are picked up on imaging), we would like to point out that lymphangiomas can also present in the adrenal and clinically and radiologically are indistinguishable from a conventional non-functional adrenal cyst.
Acknowledgements
This work has been supported by the Department of Histopathology, Guy’s & St Thomas’ Hospital, London, UK.
Footnote
Ethical Consideration: An ethical approval and/or informed consent were not required for this study.
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Ates LE, Kapran Y, Erbil Y, et al. Cystic lymphangioma of the right adrenal gland. Pathol Oncol Res 2005;11:242-4. [PubMed]
- Akand M, Kucur M, Karabagli P, et al. Adrenal lymphangioma mimicking renal cyst: a case report and review of the literature. Case Rep Urol 2013;2013:136459.
- Khoda J, Hertzanu Y, Sebbag G, et al. Adrenal cysts: diagnosis and therapeutic approach. Int Surg 1993;78:239-42. [PubMed]
- Ellis CL, Banerjee P, Carney E, et al. Adrenal lymphangioma: clinicopathologic and immunohistochemical characteristics of a rare lesion. Hum Pathol 2011;42:1013-8. [PubMed]
- Levy AD, Cantisani V, Miettinen M. Abdominal lymphangiomas: imaging features with pathologic correlation. AJR Am J Roentgenol 2004;182:1485-91. [PubMed]
- Plaut A.. Hemangiomas and related lesions of the adrenal gland. Virchows Arch Pathol Anat Physiol Klin Med 1962;335:345-55. [PubMed]
- Lin XJ, Huang CC, Cheng SM. Cystic lymphangioma of the adrenal gland: a rare case report. J Radiol Sci 2013;38:59-64.
- Garcia M, Louis LB 4th, Vernon S. Cystic adrenal lymphangioma. Arch Pathol Lab Med 2004;128:713-4. [PubMed]


