
Outcomes following minimally invasive imagine-guided percutaneous ablation of adrenal glands
Introduction
Clinically unapparent adrenal neoplasms are frequently encountered in routine practice, found in 2–10% of the population worldwide (1), and the opportunity to discover adrenal masses is constantly increasing thanks to improved sensitivity of imaging techniques (2). Among adrenal lesions, malignancies are overall rare; however, the adrenal glands are a common site for metastases, particularly from lung cancer, renal cell carcinoma (RCC), colorectal cancer, hepatocellular carcinoma (HCC), and malignant melanoma, with adrenal metastases occurring in 3–27% of cancer patients as reported by autopsy reviews (3).
Metastatic involvement of the adrenal glands is generally treated conservatively, depending on the primary malignancy, by chemotherapy or radiation therapy; however, surgery for local control has been controversial, and several reports have described the utility of open surgical or laparoscopic resection in terms of prolonged survival in selected patients with isolated metastatic disease to the adrenal glands (4,5). Nonetheless, few patients are usually eligible for surgery because of multiple comorbidities, elder age, difficult approach due to altered anatomical planes and fibrosis for previous surgery, or concomitant extra-adrenal cancer.
In recent years, the drive behind the general trend toward minimally invasive procedures represents the result of a diverse combination of factors, primarily the obvious drawbacks of almost any surgical intervention, the development and refinement of new technologies, the aim to reduce peri-operative complications and post-operative recovery time especially in subjects debilitated or who refuse surgery, and patient awareness of emerging therapeutic approaches. Image-guided ablation techniques, successfully employed in diverse clinical scenarios, have been used also for the treatment of malignant adrenal masses. The purpose of this article was to analyse the current evidence on image-guided ablative procedures for malignant adrenal neoplasms in terms of safety and outcomes.
Materials and methods/search strategy
An extended systematic search in Medline database (via PubMed), including articles related to human medicine was performed. Keywords were chosen according to Medical Subject Heading (MeSH) terms: “adrenal glands”, “adrenal gland neoplasms”, “ablation techniques”, used in combination with the Boolean operators OR and AND respectively.
The bibliographic search provided a total number of 164 citations; two independent reviewers (A.C. and F.P.) screened the initial search results considering titles and abstracts. Both reviewers had experience in data extraction for retrospective and prospective studies. Articles addressing an issue pertinent to ablation of adrenal gland malignant lesions and reporting outcome data were considered potentially eligible for inclusion. In more detail, inclusion criteria were as follows: English-written, human studies dealing with ablation techniques [namely radiofrequency ablation (RFA), microwave ablation (MWA), laser-induced interstitial thermotherapy (LITT), cryoablation (CRA), chemical ablation] used for adrenal gland primary malignancies or metastases, with consideration of outcomes of the procedures; case series of more than 3 patients. Reviews, case reports and studies which did not perform outcome analysis were excluded. All the articles selected by at least one of the reviewers were retrieved for full text evaluation and were jointly discussed to obtain an agreement in case of uncertainty. Additional searches of their reference lists were performed to identify other potentially eligible articles. Data were consequently extracted using an extraction form designed for the purpose. Finally, 20 articles were considered relevant for the aims of the literature review and were therefore included in this work (Table S1).
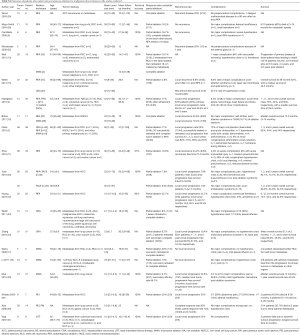
Full table
When indicated, technical and clinical successes, disease free-survival and overall survival were reported. Moreover, also complications were reported. These outcomes were defined as follows:
Technical success
The definition of technical success varies among different studies. In most studies, technical success rate, was defined as the completion of adrenal ablation according to the planned treatment protocol (6).
Clinical success
Complete ablation was generally defined as no evidence of enhancing tissue in the treated adrenal gland at post-procedural imaging or at the first follow-up, and this means successful local control of disease; the visualization of any focal area of enhancement in the ablated lesion should be deemed as residual viable tumor at imaging evaluation performed 1 month after the procedure (7).
Local disease progression or recurrence was generally identified as the appearance at follow-up imaging (more frequently CT performed after 3 months from the procedure) of new enhancing nodules at the site of a previously treated lesion (7).
Progression-free survival
Progression-free survival was defined as the length of time after treatment during which a patient survives with no sign of the disease (3,7).
Overall survival
Overall survival was defined as the length of the time after treatment and the death of the patient from any cause (7).
Safety
All complications were recorded and classified as minor and major; they were assessed according to CTCAE (8). Major complications were defined as complications that, if left untreated, might threaten the patient’s life, lead to substantial morbidity and disability, result in hospital admission or substantially lengthen hospital stay, as described by the International Working Group of Image Guided Tumour Ablation (7). Minor complications included typical post-ablation syndrome symptoms (fever, pain, nausea and vomiting) if present >4 days after the ablation procedure.
Complications were further divided into two causal categories: those secondary to device placement (pneumothorax, infection and bleeding) and in cases of thermal ablation, those secondary to thermal injury (damage to adjacent organs) (9). Hypertensive crisis (HC) is related to parenchyma destruction (10). HC has been defined as an increase of systolic blood pressure greater than 180 mmHg or an increase in diastolic pressure greater than 120 mmHg (10).
Results
Radiofrequency ablation (RFA)
Technical success, when reported, is high, ranging from 93% to 100%.
In two cases (11,12) the procedure was terminated before complete ablation because the patients developed HC during the manoeuvre, requiring adequate medical treatment; in one case (12) the ablation was suspended due to frequent ventricular fibrillation and consequent transient myocardial ischemia.
The response rate in terms of complete/partial ablation after the first session varies among the collected series, ranging from 77.3% to 100%; most residual tumors underwent repeated ablation sessions (2,3,6,12,13). Among different series collected, recurrence rate reported was up to 25% (3).
Major complications occurred in 0 to 12% of patients in different studies with inhomogeneous cohorts; these encompasses HC with myocardial ischemia (3,13,14), post-ablation syndrome, deep vein thrombosis leading to subsequent haemorrhage and splenectomy (15), acute renal failure, haemorrhage, heart failure, stroke (2), haemobilia and acute cholecystitis (3), massive pneumothorax (14), and arrhythmia (12). HC has a frequency up to 57% (3).
Overall survival rate at 3-year, when reported, ranges between 34% and 53%, with a mean follow-up of 26.3 to 37 months.
Microwave ablation (MWA)
Technical success is not reported.
MWA exerts a high local control rate with complete ablation after the first treatment session which varies between the collected series from 80% to 100%; partially ablated nodules were successfully retreated to total response with further ablative sessions in all cases (3,15-19).
Local recurrence rates are below 25% (3,16,20).
Botsa et al. (16) have found rates of local recurrence at 3-month and 1-year follow-up of 19.4%. In their study, lesions treated successfully with a single ablation were smaller than 3 cm in size, while patients who needed an additional session had a tumor diameter larger than 3 cm (16). Similar results have been found by Men and colleagues (20), reporting local recurrence rate for smaller tumors (i.e., with diameter ≤3.5 cm) significantly lower than that for greater lesions.
No major complications were reported by two out of three series describing MWA for adrenal tumors (17,19). HC was registered with a rate of 5.6% (2/31) (20). Other frequent reported minor complications are pain, post-ablation syndrome, and mild hypertension (17,19).
Survival data are limited; studies dealing with the treatment of adrenal gland metastases from lung cancer report median overall survival time of 14.6 months and 12 months (16,20). During the follow-up, patients died due to the general progression of the tumor.
Laser-induced interstitial thermotherapy (LITT)
Technical success is not reported.
Vogl et al. (21) have reported the use of CT-guided and MR-thermometry-controlled LITT in a small series of 9 patients presenting single adrenal gland nodules. Complete ablation was achieved in a single session for each tumor, producing a volume of necrosis with a mean diameter of 4.5 cm. After a mean follow-up of 10 months, 2 (22%) tumors demonstrated recurrence at the treated site; two patients died during the follow-up duration for systemic tumor progression.
There were no procedure-related complications.
Cryoablation (CRA)
Technical success is not reported.
The response rate in terms of complete/partial ablation after the first ablation is high (90.3% to 92%); moreover, patients with residual disease were all successfully retreated in subsequent CRA sessions.
No major complications were reported in the 2 series analysed (22,23). Welch et al. (24) reported HC in 46% of the cases. Other minor complications included pleural effusion and back pain.
Overall survival rate is reported only by Welch et al. (24). One-, 3-, and 5-year survival rates were 83.9%, 45.0%, and 30.0% respectively; the presence of concomitant extra-adrenal disease was a poor prognostic factor, whereas they could not find any association between primary tumor histology and survival.
Chemical ablation
Technical success is not reported.
Xiao et al. (25) treated 20 metastases in 14 patients. Percutaneous ablation was repeated an average of three times for small lesions and five for larger ones. The complete response rate was 30% at 24-month follow-up, whereas a partial response to treatment was verified in the remaining 70% of cases.
In the treatment of malignant lesions, Shibata and colleagues (26) ablated 9 metastases from HCC in 7 patients with two to four sessions per lesion. Post-procedural CT showed residual enhancing tissue in two lesions (22%), which were bilateral metastases in the same patient. During the follow-up (6–36 months), 3 nodules (33%) were further increased in size, while the remaining were not; after 6–28 months, one patient died from liver failure, and two from extra-adrenal metastatic spread.
No major complications were registered in the 2 reported studies. Fever and pain were the most common adverse events, and one patient experienced adrenal insufficiency (25,26).
About 35.7% of patients died at 2 years due to extra-adrenal disease progression in the series reported by Xiao et al. (25).
Discussion
Surgical resection, whenever possible, represents the gold standard for primary adrenal neoplasm treatment; conversely, surgery for local control in patients with adrenal metastases is still controversial in the literature. In patients who are poor surgical candidates or who refuse surgery, percutaneous image-guided ablation may be considered a valid alternative.
The best treatment strategy must be decided by a multidisciplinary team including the interventional radiologist, oncologist, surgeon, and endocrinologist (27,28), considering risks and benefits for patients with several comorbidities.
Besides the concerns of patient selection, tumor size represents a relevant factor to be considered while attempting to achieve complete tumor ablation: it seems clear that the smaller is the maximum diameter, the greater the likelihood of a successful complete ablation. Although a consensus has not been achieved yet on a threshold size, better results have been reported for adrenal masses smaller than 5 cm (3,29,30). Other investigators reported a lower threshold, i.e., 4 (22) or even 3 cm for lesions successfully treated with a single ablative session (11,16), or to prevent local tumor progression (2).
General contraindications to adrenal ablative therapy are similar to the contraindications of the same procedures applied to other organs. For instance, as with any image-guided procedure, the risk of haemorrhage must be taken into account; therefore coagulopathies should be corrected before the ablation, and the international normalized ratio (INR) should be less than 1.5 and platelet count greater than 50,000/µL (27).
In addition to careful access planning based on imaging assessment, some investigators have reported that preprocedural or periprocedural adrenergic blockade may need to be implemented with the aim to prevent HC (13,15) in cases of nonfunctional tumors due to the sudden release into the systemic circulation of catecholamines normally stored in the adrenal medulla surrounding the tumor (23), and in cases of functional tumors this indication reflects guidelines on pheochromocytomas in the surgical literature (31). Fintelmann and colleagues (23) reported in their series a lower likelihood of HC in tumors greater than 4.5 cm with no visible viable gland; hence, preprocedural imaging may be also useful to estimate the risk of the most serious and relatively common side effect of otherwise well-tolerated procedures.
On the other hand, some reports have suggested that α-blockade may not be routinely needed, as most of the HCs encountered were well-controlled after adequate medical treatment (11).
RFA is the most used ablative technique described in literature for the percutaneous treatment of adrenal lesions. Most articles collected for the literature review deal with RFA of adrenal metastases from RCC, lung carcinoma, HCC, melanoma, gastrointestinal tumors and other malignancies; however, RFA has been used to treat not only metastatic tumors but also primary and metastatic adrenocortical carcinomas (ACC) (30).
Mayo-Smith et al. (29) have described the use of RFA in adrenal gland metastasis treatment. They found that the average size of the two adrenal masses that demonstrated viable residual tumor after ablation was 6.0 cm, compared with 3.6 cm for completely ablated lesions, but this difference was not significant.
In fact, the size of the lesion to be treated is a significant predictor of residual disease after ablation. Recently, Zhou et al. (14) found that patients with residual tumor had significantly larger nodules, and identified the threshold of 3 cm to predict the likelihood of incomplete ablation. This finding may be explained by the local effect of RFA in tumor thermal damage, since only lesions limited in size [i.e., with a diameter smaller than 4 cm (6)] can be ablated with each application depending on the electrode type.
Accordingly, Hasegawa et al. (2) confirmed the threshold of 3 cm to be a significant factor affecting local tumor progression.
Comparing transarterial embolization (TACE) alone with a combination treatment of TACE with simultaneous RFA, Yuan et al. (32) concluded that the second strategy led to a better local control of adrenal metastases from HCC (75.0% of patients) compared with TACE alone (35.3%) at the last follow-up assessment.
Really few data are available about the role of CRA; the results described outlined similar effectiveness to other thermal techniques employed for the same purpose, and local control rate (80.6%) was comparable to that of surgery (77–83%) (23).
Chemical ablation was considered a poor alternative in bilateral and large metastases (>5 cm in diameter), in which thermal ablation techniques may produce better results in terms of disease local control (32).
Few studies have analysed the benefits in terms of survival of adrenal ablation, because of small and inhomogeneous patient cohorts, different techniques applied, and short-term follow-up; moreover, it should be borne in mind that the eventual prognosis of patients strongly depends on the primary malignancy. This makes it difficult to compare the results from different series featuring adrenal ablation.
Frenk et al. (3), describing use of RFA, CRA and MWA to treat 46 adrenal metastases, indicated a median overall survival of 30 months, which was significantly worse in patients with non-small cells lung cancer (NSCLC), which was found a significant predictor of worse outcome. In the whole population, local control and overall survival at 2 years compared favourably with results of surgical removal based on a systematic review of the literature (33).
Age of 65 years or older and the presence of extra-adrenal tumors were also identified to be worse prognostic factors (2) in patients with adrenal metastases. Whether the first prognostic determinant is obvious, the latter may be explicated thanks to the higher disease stage even after RF ablation in subjects presenting concomitant extra-adrenal disease.
Another retrospective study (16) included 71 patients with single adrenal metastases from NSCLC, treated by RFA (n=35) or MWA (n=36); the investigators revealed a median overall survival time of 14.0 months, with no significant difference in survival between the two different technique groups.
The aforementioned work by Yuan and colleagues (32) suggested that a combined therapy for adrenal metastases from HCC may be more effective than TACE alone: the overall survival rate was significantly higher in the group of patients receiving TACE+RFA therapy than in the TACE alone group (at 3 years 55.3% vs. 44.0%), in spite of more complications related to RFA usage that were shown to easily resolve after active management.
Percutaneous image-guided techniques are safe and well-tolerated procedure; HC is the most frequent complication reported. However, most cases were successfully treated by prompt medical intervention, and ablations were successfully completed (6). The risk of sudden blood pressure increase is greater during treatment of tumors adjacent to viable adrenal parenchyma than during ablation of larger tumors localized in a gland completely occupied by the lesion (23).
There is disagreement about the role of MWA in inducing HC: some authors have suggested that the rapid rise in temperature may produce such complication more frequently than RFA, due to an excessive release of catecholamines; conversely, other investigators have reported that the risk with MWA could be lower, due to the shorter application time (18,19,24).
Welch et al. (24) and Zhang et al. (34) performed a hemodynamic change analysis during percutaneous adrenal CRA, and concluded that these patients should be pharmacologically pre-treated in a way similar to patients undergoing surgery for pheochromocytoma.
Others minor complications more frequently encountered included pain, post-RFA syndrome, minimal pneumothorax, transient urinary retention or bleeding, reduced renal function, retroperitoneal abscess, small haematoma, and transient arrhythmia, as shown in Table S1.
Conclusions
Percutaneous image-guided ablation for primary and metastatic malignancies of the adrenal glands is feasible and safe, with zero mortality and negligible morbidity. Currently, there are no large randomized controlled trials which demonstrate the efficacy of this treatment strategy in terms of local progression and survival, compared with surgical removal. However, percutaneous ablation is a useful therapeutic option for controlling unresectable adrenal metastases, offering patients opportunities for improved survival.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Özer Makay) for the series “Robotic Adrenalectomy” published in Gland Surgery. The article was sent for external peer review organized by the Guest Editor and the editorial office.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/gs.2020.03.32). The series “Robotic Adrenalectomy” was commissioned by the editorial office without any funding or sponsorship. SAA serves as an unpaid editorial board member of Gland Surgery from June 2019 to May 2021. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Crona J, Beuschlein F, Pacak K, et al. Advances in adrenal tumors 2018. Endocr Relat Cancer 2018;25:R405-20. [Crossref] [PubMed]
- Hasegawa T, Yamakado K, Nakatsuka A, et al. Unresectable Adrenal Metastases: Clinical Outcomes of Radiofrequency Ablation. Radiology 2015;277:584-93. [Crossref] [PubMed]
- Frenk NE, Daye D, Tuncali K, et al. Local Control and Survival after Image-Guided Percutaneous Ablation of Adrenal Metastases. J Vasc Interv Radiol 2018;29:276-84. [Crossref] [PubMed]
- Puccini M, Panicucci E, Candalise V, et al. The role of laparoscopic resection of metastases to adrenal glands. Gland Surg 2017;6:350-4. [Crossref] [PubMed]
- Paul CA, Virgo KS, Wade TP, et al. Adrenalectomy for isolated adrenal metastases from non-adrenal cancer. Int J Oncol 2000;17:181-7. [PubMed]
- Carrafiello G, Laganà D, Recaldini C, et al. Imaging-guided percutaneous radiofrequency ablation of adrenal metastases: Preliminary results at a single institution with a single device. Cardiovasc Intervent Radiol 2008;31:762-7. [Crossref] [PubMed]
- Ahmed M, Solbiati L, Brace CL, et al. Image-guided Tumor Ablation: Standardization of Terminology and Reporting Criteria—A 10-Year Update. Radiology 2014;273:241-60. [Crossref] [PubMed]
- The National Cancer Institute. Common Terminology Criteria for Adverse Events (CTCAE) v4.0. 2010.
- Rhim H, Dodd GD, Chintapalli KN, et al. Radiofrequency Thermal Ablation of Abdominal Tumors: Lessons Learned from Complications. Radiographics 2004;24:41-52. [Crossref] [PubMed]
- Chobanian AV, Bakris GL, Black HR, et al. Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003;42:1206-52. [Crossref] [PubMed]
- Zhou K, Pan J, Yang N, et al. Effectiveness and safety of CT-guided percutaneous radiofrequency ablation of adrenal metastases. Br J Radiol 2018;91:20170607. [Crossref] [PubMed]
- Huang J, Xie X, Lin J, et al. Percutaneous radiofrequency ablation of adrenal metastases from hepatocellular carcinoma: a single-center experience. Cancer Imaging 2019;19:44. [Crossref] [PubMed]
- Wolf FJ, Dupuy DE, Machan JT, et al. Adrenal neoplasms: Effectiveness and safety of CT-guided ablation of 23 tumors in 22 patients. Eur J Radiol 2012;81:1717-23. [Crossref] [PubMed]
- Zhou W, Herwald SE, Uppot RN, et al. Image-Guided Thermal Ablation for Non-resectable Recurrence of Renal Cell Cancer Following Nephrectomy: Clinical Experience with Eleven Patients. Cardiovasc Intervent Radiol 2018;41:1743-50. [Crossref] [PubMed]
- Welch BT, Callstrom MR, Carpenter PC, et al. A Single-Institution Experience in Image-Guided Thermal Ablation of Adrenal Gland Metastases. J Vasc Interv Radiol 2014;25:593-8. [Crossref] [PubMed]
- Botsa EI, Thanou IL, Papatheodoropoulou AT, et al. Thermal ablation in the management of adrenal metastasis originating from non-small cell lung cancer: A 5-year single-center experience. Chin Med J 2017;130:2027-32. [Crossref] [PubMed]
- Wang Y, Liang P, Yu X, et al. Ultrasound-guided percutaneous microwave ablation of adrenal metastasis: Preliminary results. Int J Hyperthermia 2009;25:455-61. [Crossref] [PubMed]
- Venkatesan AM, Locklin J, Dupuy DE, et al. Percutaneous Ablation of Adrenal Tumors. Tech Vasc Interv Radiol 2010;13:89-99. [Crossref] [PubMed]
- Li X, Fan W, Zhang L, et al. CT-guided percutaneous microwave ablation of adrenal malignant carcinoma: Preliminary results. Cancer 2011;117:5182-8. [Crossref] [PubMed]
- Men M, Ye X, Fan W, et al. Short-term outcomes and safety of computed tomography-guided percutaneous microwave ablation of solitary adrenal metastasis from lung cancer: A multi-center retrospective study. Korean J Radiol 2016;17:864-73. [Crossref] [PubMed]
- Vogl TJ, Lehnert T, Eichler K, et al. Adrenal metastases: CT-guided and MR-thermometry-controlled laser-induced interstitial thermotherapy. Eur Radiol 2007;17:2020-7. [Crossref] [PubMed]
- Mouracade P, Dettloff H, Schneider M, et al. Radio-frequency Ablation of Solitary Adrenal Gland Metastasis From Renal Cell Carcinoma. Urology 2009;74:1341-3. [Crossref] [PubMed]
- Fintelmann FJ, Tuncali K, Puchner S, et al. Catecholamine Surge during Image-Guided Ablation of Adrenal Gland Metastases: Predictors, Consequences, and Recommendations for Management. J Vasc Interv Radiol 2016;27:395-402. [Crossref] [PubMed]
- Welch BT, Atwell TD, Nichols DA, et al. Percutaneous image-guided adrenal cryoablation: Procedural considerations and technical success. Radiology 2011;258:301-7. [Crossref] [PubMed]
- Xiao YY, Tian JL, Li JK, et al. CT-guided percutaneous chemical ablation of adrenal neoplasms. AJR Am J Roentgenol 2008;190:105-10. [Crossref] [PubMed]
- Shibata T, Maetani Y, Ametani F, et al. Percutaneous ethanol injection for treatment of adrenal metastasis from hepatocellular carcinoma. AJR Am J Roentgenol 2000;174:333-5. [Crossref] [PubMed]
- Ierardi AM, Petrillo M, Patella F, et al. Interventional radiology of the adrenal glands: Current status. Gland Surg 2018;7:147-65. [Crossref] [PubMed]
- Yamakado K. Image-Guided Ablation of Adrenal Lesions. Semin Intervent Radiol 2014;31:149-56. [Crossref] [PubMed]
- Mayo-Smith WW, Dupuy DE. Adrenal Neoplasms: CT-guided Radiofrequency Ablation—Preliminary Results. Radiology 2004;231:225-30. [Crossref] [PubMed]
- Wood BJ, Abraham J, Hvizda JL, et al. Radiofrequency ablation of adrenal tumors and adrenocortical carcinoma metastases. Cancer 2003;97:554-60. [Crossref] [PubMed]
- Pacak K, Lenders JWM, Eisenhofer G. Pheochromocytoma: Diagnosis, Localization, and Treatment. Oxford, UK: Blackwell Publishing Ltd, 2007.
- Yuan H, Liu F, Li X, et al. Clinical efficacy of chemoembolization with simultaneous radiofrequency ablation for treatment of adrenal metastases from hepatocellular carcinoma. Cancer Imaging 2018;18:24-8. [Crossref] [PubMed]
- Gunjur A, Duong C, Ball D, et al. Surgical and ablative therapies for the management of adrenal ‘oligometastases’ - A systematic review. Cancer Treat Rev 2014;40:838-46. [Crossref] [PubMed]
- Zhang W, Sun LJ, Xu J, et al. Computed tomography-guided cryoablation for adrenal metastases: local control and survival. Medicine 2018;97:e13885. [Crossref] [PubMed]


