Nipple-areolar complex reconstruction and patient satisfaction: a systematic review and meta-analysis
Introduction
Nipple-areola complex (NAC) reconstruction traditionally marks the final stage of breast reconstruction following mastectomy, making it an important component of the multidisciplinary approach to breast cancer. Many women endorse that the presence of a nipple following mastectomy improves body image and decreases the sense of mutilation that can accompany a mastectomy. Although preservation of a patient’s native nipple using a nipple-sparing mastectomy (NSM) technique may obviate this reconstructive step (1-8), it is sometimes not an option for patients from an oncologic perspective.
In the case of a unilateral mastectomy, composite nipple sharing can often provide a symmetric, satisfactory result (9,10). More often, however, local tissue rearrangement is used to create a nipple, followed by tattooing of the reconstructed nipple and the surrounding skin that is to become the areola. A variety of local flaps has been described in the literature (1,9-23).
Given that the benefit of breast and nipple reconstruction is aimed at psychosocial well-being rather than disease treatment, patient satisfaction is the most important outcome assessment measure. While separate studies exist that evaluate patient satisfaction with NSM and individual NAC reconstructive techniques, there is a lack of literature offering comparison between the level of satisfaction with the different methods of NAC reconstruction described and between NAC reconstruction and NSM among women undergoing mastectomy. This systematic review and meta-analysis sought to provide such comparisons.
Methods
This systematic review and meta-analysis was conducted in accordance with the preferred reporting items for systematic reviews and meta-analysis (PRISMA) guidelines (24).
Systematic review
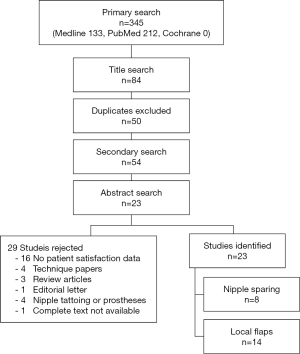
A literature search was conducted using the U.S. National Library of Medicine (MEDLINE), PubMed and the Cochrane Database to identify relevant English (language) articles published between 1992 and March 2012. Keywords “nipple reconstruction” and “patient satisfaction” were used. Medical subject heading (MeSH) terms “nipples”, “reconstructive surgical procedures”, “satisfaction” and “sensation” were also exploded. Resulting article titles were examined for relevance, and duplicate title were excluded. A secondary search was conducted by evaluating references of all primary articles for any additional relevant studies. Article abstracts, and when necessary full text, were then reviewed for relevance. Exclusion criteria included technique papers, case reports and reviews. To facilitate comparison, only articles including quantitative measures of patient satisfaction were utilized. Articles were then classified based on nipple reconstructive technique—either composite nipple sharing or local flap reconstruction, with NSM used as a control. This article selection process is detailed in Figure 1.
Quality of evidence
Each selected study was reviewed using the GRADE approach to assess the confidence in its estimate of effect. This included an assessment of the risk of bias and validity of the patient-report outcome measure used.
Data extraction and analysis
Given that a variety of aspects of patient satisfaction were evaluated with different measures used as a mark of satisfaction, a method of determining a standardized “Satisfaction Score” (SS) for the most commonly reported data points for each reconstructive method was used for the purpose of this review. A SS for both “nipple appearance” and “nipple sensation” was calculated for local flap reconstruction, as well as NSM as a control. No SS was calculated for composite nipple sharing as too few data points were identified.
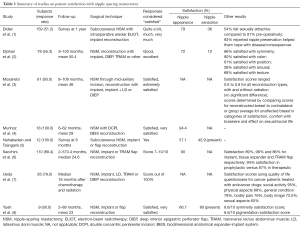
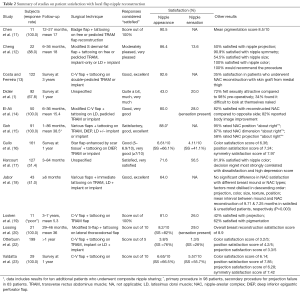
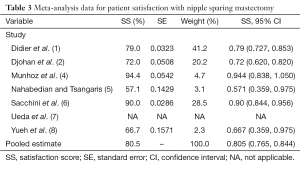
The majority of studies used patient surveys with Likert scale response choices. The SS for such data was determined as the percentage of patients providing a satisfactory response as designated in the article text or decided by the reviewers. For example, many studies designated “satisfied” or “very satisfied” as survey responses indicating that the patient was satisfied. For studies utilizing a numerical scale where patients selected an integer on a scale of 1 to 5 or 1 to 10 to indicate their satisfaction, the percentage of patients providing numerical responses deemed to indicate satisfaction as described by the authors was used as the SS. In studies providing only an average numerical satisfaction value, that value was converted to a percentage by dividing by the total possible score. For example, an average satisfaction value of 3.5 on a scale of 1 to 5 translated to an SS of 70%. Similarly, for surveys asking patients to report their overall satisfaction as a percentage, the average percentage reported was used as the SS. The type of data used to determine the SS for each study is detailed in Tables 1,2. The overall SS for local flap reconstruction and NSM was determined by calculating an average SS weighted by the number of subjects in each study as shown in Tables 3,4.
Full table
Full table
Full table

Full table
Data analysis also included a Fisher’s exact test to determine if there was a statistically significant difference between the SS with local flap reconstruction compared to that with NSM, as well as between the individual local flap reconstruction techniques compared to all other flap techniques combined.
Results
Data extraction and analysis
Initial primary search identified 345 articles with four additional articles found in the secondary search of the references from relevant articles. Of these, a total of 23 studies met the systematic review inclusion criteria, all containing patient satisfaction data. For use as a control, eight articles examining satisfaction with nipple-sparing mastectomies on 473 patients were included. Two articles evaluating the use of composite nipple sharing in 91 patients were identified. Fourteen studies contained satisfaction data from 984 patients undergoing nipple reconstruction with various local skin flaps.
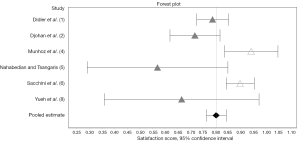
For each included article, the number of subjects, length of follow-up, surgical technique and patient satisfaction data was determined and recorded in Tables 1,2,5. Table 1 reflects data from patients undergoing NSM with various methods of reconstruction including both immediate and staged implants, as well as pedicled and free autologous flaps. Of the nine NSM articles identified, six contained patient satisfaction data for nipple appearance from 386 patients. The weighted average SS was 80.5% (95% CI, 0.765–0.844) as calculated in Table 3 and shown in Figure 2. Only two studies included satisfaction data for nipple sensation from 237 patients, which yielded a weighted average SS of 27.4%.
Full table
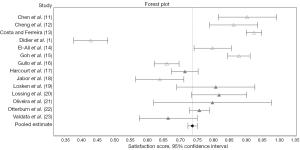
The data from articles evaluating the use of local skin flap reconstruction is shown in Table 2. The most commonly used local flap techniques included C-V, S, star, skate and badge flaps, with or without modification. All 14 included studies contained data for calculation of an SS for nipple appearance; the weighted average SS was 73.9% (95% CI, 0.725–0.753) as calculated in Table 4 and shown in Figure 3. Seven of the articles provided nipple sensation satisfaction data with a weighted average SS of 35.9%. The studies with the highest reported SS for appearance were those which used the C-V and badge local flap techniques with a SS of 92.6% and 90.5%, respectively.
A Fisher’s exact test comparing patient satisfaction with local flap reconstruction compared to NSM had a P value of 0.0079. A significant difference in SS (P=0.0001) was also seen in studies which utilized only a C-V or modified C-V flap technique compared to those using one or more other flap techniques.
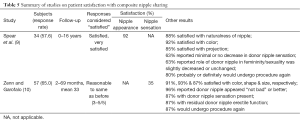
Only one of the two nipple sharing studies provided results for each nipple appearance and nipple sensitivity (Table 5). For this reason, no SS was calculated for either category.
Quality of evidence
Using the GRADE approach, the studies were evaluated for the confidence in their estimate of effect. As no widely-accepted, validated questionnaire for nipple reconstruction satisfaction exists, the validity of patient-reported outcome measures utilized cannot be established. All 23 included studies were performed retrospectively and relied on patient questionnaire responses, making them inherently prone to response bias. The eight studies with response rates less than 80% were considered to be at higher risk of bias due to low response rates. There were also four studies which did not disclose a response rate. A lower confidence was also attributed to studies of smaller size. In reviewing the collection of studies as a whole, a great deal of publication bias is likely also present due to the reluctance to report low patient satisfaction results.
Discussion
Breast reconstruction has become a fundamental component of the multidisciplinary approach toward the treatment of women with breast cancer, making the plastic surgeon an integral part of this treatment team. The breast is an important component of the female identity. Following mastectomy, women report that undergoing reconstruction helps them to feel as though they have overcome the disease, to cope with their feelings regarding the loss of their breast and to improve their body image (25).
Previous studies assessing patient satisfaction with various methods of breast reconstruction have established that the presence of a nipple, whether native or reconstructed, positively impacts overall patient satisfaction with the breast. Posited explanations include the creation of a finished looking breast, an increased sense of attractiveness, a feeling of a more normal appearance and improvement in symmetry in cases of unilateral reconstruction (18,26-29).
Given that both breast mound and nipple reconstruction play a psychosocial, rather than a disease-modification role, patient satisfaction and health-related quality of life (HR-QoL) improvement are the most important outcomes of interest. Assessment of these outcome measures, however, is subjective and difficult to evaluate. It relies on the use of patient surveys and questionnaires which introduce response and self-selection bias. In a systematic review such as this, further difficulty exists due to the lack of consistency in the manner in which “satisfaction” is measured, both in the aspects of the reconstruction evaluated and the quantification of the responses. The ability to draw conclusions based on the statistical results of this review is extremely limited by the created SS. While we feel this was the best available method to allow comparison between the included studies, it was clearly less than ideal.
The utilization of standardized patient-reported outcome measures like the BREAST-Q provides a way to quantify patient satisfaction and HR-QoL outcomes (29). Currently, this type of validated outcome measure does not exist specifically for nipple reconstruction, but it would be beneficial in providing surgeons a tool to assess their own outcomes and facilitate comparison between the many different local flap techniques. It would also allow for more consistency when assessing multiple different studies or conducting multi-center studies.
Despite the imperfect comparative analysis technique utilized due to the limitations of the available publications, a significantly higher patient SS was seen with use of the C-V or modified C-V flap. Reasons authors cited for favoring this flap included its ease, consistency, reliability and lack of donor site morbidity (14,19,22,23). With the high satisfaction seen regardless of technique, however, factors such as surgeon preference and experience should be considered when choosing a nipple reconstruction technique.
As the oncologic safety of nipple-sparring mastectomy continues to be better understood and accepted, more and more patients will likely be able to keep their native nipples. There will, however, always be cases in which resection of the NAC is necessary, making ever-relevant the quest for an ideal nipple reconstruction technique that provides a realistic, well-projected nipple with a high patient satisfaction rate.
Conclusions
Patient satisfaction with nipple reconstruction is high, regardless of the technique used. Although patient satisfaction with breast reconstruction has previously been demonstrated to be higher with nipple reconstruction compared to foregoing nipple reconstruction, patient satisfaction is significantly higher among those who undergo NSM than those who require nipple reconstruction with one of a variety of popular local flap techniques. When safe from an oncologic perspective, NSM should be performed when possible. When NSM is not an option, local flap reconstruction with C-V or modified C-V flap may be associated with higher satisfaction than alternative local flap techniques.
Acknowledgements
None.
Footnote
Conflicts of Interest: Dr. Nahabedian is a speaker/consultant for LifeCell, Sientra, and Allergan. Dr. Satteson and Dr. Brown have no conflicts of interest to declare.
References
- Didier F, Radice D, Gandini S, et al. Does nipple preservation in mastectomy improve satisfaction with cosmetic results, psychological adjustment, body image and sexuality? Breast Cancer Res Treat 2009;118:623-33. [Crossref] [PubMed]
- Djohan R, Gage E, Gatherwright J, et al. Patient satisfaction following nipple-sparing mastectomy and immediate breast reconstruction: an 8-year outcome study. Plast Reconstr Surg 2010;125:818-29. [Crossref] [PubMed]
- Mosahebi A, Ramakrishnan V, Gittos M, et al. Aesthetic outcome of different techniques of reconstruction following nipple-areola-preserving envelope mastectomy with immediate reconstruction. Plast Reconstr Surg 2007;119:796-803. [Crossref] [PubMed]
- Munhoz AM, Aldrighi C, Montag E, et al. Optimizing the nipple-areola sparing mastectomy with double concentric periareolar incision and biodimensional expander-implant reconstruction: aesthetic and technical refinements. Breast 2009;18:356-67. [Crossref] [PubMed]
- Nahabedian MY, Tsangaris TN. Breast reconstruction following subcutaneous mastectomy for cancer: a critical appraisal of the nipple-areola complex. Plast Reconstr Surg 2006;117:1083-90. [Crossref] [PubMed]
- Sacchini V, Pinotti JA, Barros AC, et al. Nipple-sparing mastectomy for breast cancer and risk reduction: oncologic or technical problem? J Am Coll Surg 2006;203:704-14. [Crossref] [PubMed]
- Ueda S, Tamaki Y, Yano K, et al. Cosmetic outcome and patient satisfaction after skin-sparing mastectomy for breast cancer with immediate reconstruction of the breast. Surgery 2008;143:414-25. [Crossref] [PubMed]
- Yueh JH, Houlihan MJ, Slavin SA, et al. Nipple-sparing mastectomy: evaluation of patient satisfaction, aesthetic results, and sensation. Ann Plast Surg 2009;62:586-90. [Crossref] [PubMed]
- Spear SL, Schaffner AD, Jespersen MR, et al. Donor-site morbidity and patient satisfaction using a composite nipple graft for unilateral nipple reconstruction in the radiated and nonradiated breast. Plast Reconstr Surg 2011;127:1437-46. [Crossref] [PubMed]
- Zenn MR, Garofalo JA. Unilateral nipple reconstruction with nipple sharing: time for a second look. Plast Reconstr Surg 2009;123:1648-53. [Crossref] [PubMed]
- Chen SG, Chiu TF, Su WF, et al. Nipple-areola complex reconstruction using badge flap and intradermal tattooing. Br J Surg 2005;92:435-7. [Crossref] [PubMed]
- Cheng MS, Ho CM, Cheung WY, et al. Nipple-areola reconstruction in autologous breast reconstruction: Chinese patients' perspective. Ann Plast Surg 2004;53:328-33. [Crossref] [PubMed]
- Costa MP, Ferreira MC. Aesthetic quality of the nipple-areola complex in breast reconstruction with a new local graft technique. Aesthetic Plast Surg 2009;33:774-9. [Crossref] [PubMed]
- El-Ali K, Dalal M, Kat CC. Modified C-V flap for nipple reconstruction: our results in 50 patients. J Plast Reconstr Aesthet Surg 2009;62:991-6. [Crossref] [PubMed]
- Goh SC, Martin NA, Pandya AN, et al. Patient satisfaction following nipple-areolar complex reconstruction and tattooing. J Plast Reconstr Aesthet Surg 2011;64:360-3. [Crossref] [PubMed]
- Gullo P, Buccheri EM, Pozzi M, et al. Nipple reconstruction using a star flap enhanced by scar tissue: the Regina Elena Cancer Institute experience. Aesthetic Plast Surg 2011;35:731-7. [Crossref] [PubMed]
- Harcourt D, Russell C, Hughes J, et al. Patient satisfaction in relation to nipple reconstruction: the importance of information provision. J Plast Reconstr Aesthet Surg 2011;64:494-9. [Crossref] [PubMed]
- Jabor MA, Shayani P, Collins DR, et al. Nipple-areola reconstruction: satisfaction and clinical determinants. Plast Reconstr Surg 2002;110:457-63; discussion 464-5. [Crossref] [PubMed]
- Losken A, Mackay GJ, Bostwick J. Nipple reconstruction using the C-V flap technique: a long-term evaluation. Plast Reconstr Surg 2001;108:361-9. [Crossref] [PubMed]
- Lossing C, Brongo S, Holmström H. Nipple reconstruction with a modified S-flap technique. Scand J Plast Reconstr Surg Hand Surg 1998;32:275-9. [Crossref] [PubMed]
- Oliveira M, Nunes D, Beolchi M, et al. Circular local skin flap. A new approach to areola reconstruction. Acta Cir Bras 2007;22:322-6. [Crossref] [PubMed]
- Otterburn DM, Sikora KE, Losken A. An outcome evaluation following postmastectomy nipple reconstruction using the C-V flap technique. Ann Plast Surg 2010;64:574-8. [PubMed]
- Valdatta L, Montemurro P, Tamborini F, et al. Our experience of nipple reconstruction using the C-V flap technique: 1 year evaluation. J Plast Reconstr Aesthet Surg 2009;62:1293-8. [Crossref] [PubMed]
- Moher D, Liberati A, Telzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 2009;339:b2535. [Crossref] [PubMed]
- Filiberti A, Tamburini M, Murru L, et al. Psychologic effects and esthetic results of breast reconstruction after mastectomy. Tumori 1986;72:585-8. [PubMed]
- Guyomard V, Leinster S, Wilkinson M. Systematic review of studies of patients’ satisfaction with breast reconstruction after mastectomy. Breast 2007;16:547-67. [Crossref] [PubMed]
- Ramon Y, Ullmann Y, Moscona R, et al. Aesthetic results and patient satisfaction with immediate breast reconstruction using tissue expansion: a follow-up study. Plast Reconstr Surg 1997;99:686-91. [Crossref] [PubMed]
- Shaikh-Naidu N, Preminger BA, Rogers K, et al. Determinants of aesthetic satisfaction following TRAM and implant breast reconstruction. Ann Plast Surg 2004;52:465-70; discussion 470. [Crossref] [PubMed]
- Pusic AL, Klassen AF, Scott AM, et al. Development of a new patient-reported outcome measure for breast surgery: The BREAST-Q. Plast Reconst Surg 2009;124:345-53. [Crossref] [PubMed]